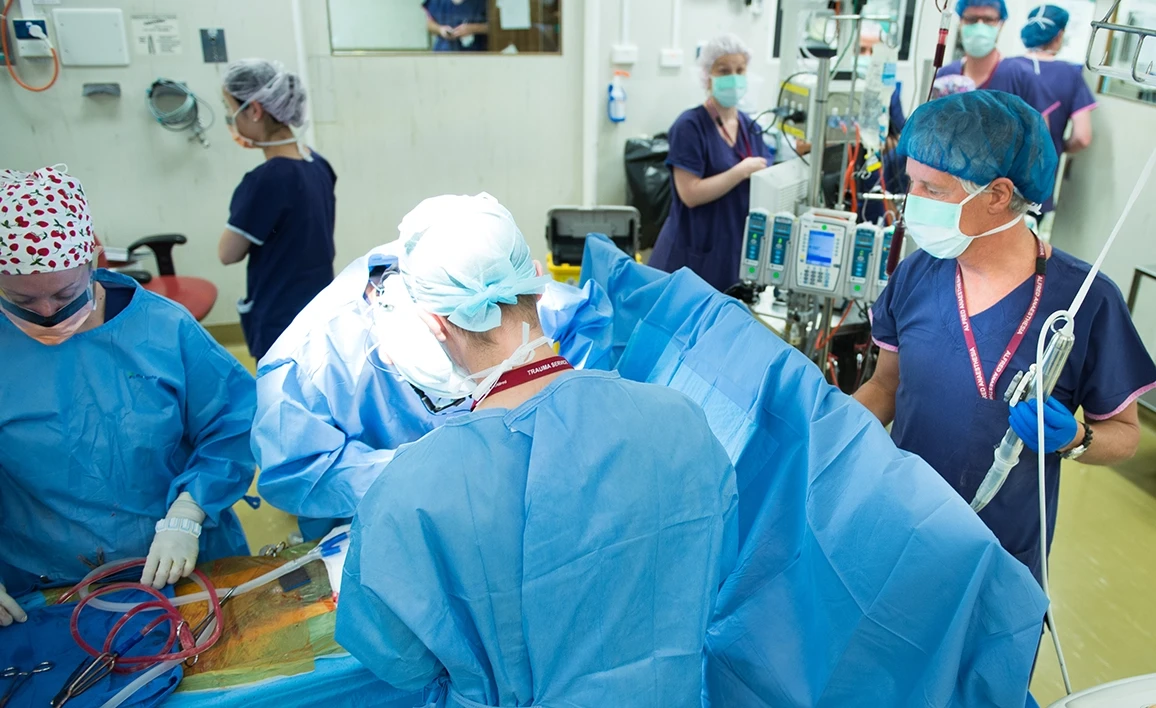
3000 patients were enrolled between May 2013 through to September 2016.
Background
Guidelines to promote the early recovery of patients undergoing major surgery recommend a restrictive intravenous-fluid strategy for abdominal surgery. However, the supporting evidence is limited, and there is concern about impaired organ perfusion.
Methods
In a pragmatic, international trial, we randomly assigned 3000 patients who had an increased risk of complications while undergoing major abdominal surgery to receive a restrictive or liberal intravenous-fluid regimen during and up to 24 hours after surgery. The primary outcome was disability-free survival at 1 year. Key secondary outcomes were acute kidney injury at 30 days, renal-replacement therapy at 90 days, and a composite of septic complications, surgical-site infection, or death.
Results
During and up to 24 hours after surgery, 1490 patients in the restrictive fluid group had a median intravenous-fluid intake of 3.7 liters (interquartile range, 2.9 to 4.9), as compared with 6.1 liters (interquartile range, 5.0 to 7.4) in 1493 patients in the liberal fluid group (P<0.001). The rate of disability-free survival at 1 year was 81.9% in the restrictive fluid group and 82.3% in the liberal fluid group (hazard ratio for death or disability, 1.05; 95% confidence interval, 0.88 to 1.24; P=0.61). The rate of acute kidney injury was 8.6% in the restrictive fluid group and 5.0% in the liberal fluid group (P<0.001). The rate of septic complications or death was 21.8% in the restrictive fluid group and 19.8% in the liberal fluid group (P=0.19); rates of surgical-site infection (16.5% vs. 13.6%, P=0.02) and renal-replacement therapy (0.9% vs. 0.3%, P=0.048) were higher in the restrictive fluid group, but the between-group difference was not significant after adjustment for multiple testing.
Conclusions
Among patients at increased risk for complications during major abdominal surgery, a restrictive fluid regimen was not associated with a higher rate of disability-free survival than a liberal fluid regimen and was associated with a higher rate of acute kidney injury.
The Australian National Health and Medical Research Council (NHMRC), the Australian and New Zealand College of Anaesthetists, Monash University, the Health Research Council of New Zealand, and the United Kingdom National Institute of Health Research.
Seed funding was received from ANZCA Research Foundation to complete the pilot study.
The RELIEF trial was the first large randomised trial evaluating perioperative IV fluid volumes, and was funded by the ANZCA Research Foundation and NHMRC.
Each year at least 310 million people undergo major surgery worldwide. All receive intravenous (IV) fluids. Clinicians have traditionally administered generous amounts of IV fluids perioperatively, to correct for preoperative fasting, blood loss and other fluid deficits. But the optimal IV fluid regimen for patients undergoing major abdominal surgery was unclear. If fluid administration is restricted it is likely that hypotension needs to be treated with vasopressors. Vasopressors may impair organ perfusion, threaten local tissues at the site of IV administration, cause arrhythmias, and be mistakenly used when hypovolaemia is the underlying cause. On the other hand, excess IV fluid administration causes tissue oedema, with increased pulmonary morbidity, impaired coagulation, and poor wound healing. Most recent guidelines, particularly those focussing on enhanced recovery after surgery, have recommended limiting IV fluid administration, aiming for a zero-balance.
The RELIEF trial was a pragmatic, multicentre, randomised, trial conducted in 47 hospitals across seven countries. A total of 3000 patients were enrolled and randomly assigned to a restrictive or liberal IV fluid regimen.
The study population consisted of at-risk patients undergoing planned major abdominal or pelvic surgery with an expected operative duration of at least two hours. The primary endpoint was disability-free survival, a novel patient-centred outcome measure. Secondary outcomes included 30-day acute kidney injury, a composite of septic complications, surgical site infection or death, and 90-day renal replacement therapy.
The findings of the study surprised many: although the two groups of patients had similar disability-free survival at one year, those in the restrictive group had a higher risk of acute kidney injury, surgical site infection, and need for renal replacement therapy after surgery. Accordingly, the authors recommended that a moderately liberal approach to perioperative IV fluid therapy for patients undergoing major abdominal surgery.
ClinicalTrials.gov number, NCT01424150.
Myles PS, Bellomo R, Corcoran T, Forbes A, Peyton P, Story D, Christophi C, Leslie K, McGuinness S, Parke R, Serpell J, Chan MTV, Painter T, McCluskey S, Minto G, Wallace S; Australian and New Zealand College of Anaesthetists Clinical Trials Network and the Australian and New Zealand Intensive Care Society Clinical Trials Group. Restrictive versus Liberal Fluid Therapy for Major Abdominal Surgery. N Engl J Med. 2018 Jun 14;378(24):2263-2274. doi: 10.1056/NEJMoa1801601. Epub 2018 May 9. PMID: 29742967.
Presentations were made by the study principal investigator, Professor Paul Myles at the ANZCA Annual Scientific Meeting in Sydney in 2016.
Australia, New Zealand, United Kingdom, United States of America, Canada and Hong Kong.
Myles PS, Bellomo R, Corcoran T, Forbes A, Wallace S, Peyton P, Christophi C, Story D, Leslie K, Serpell J, McGuinness S, Parke R; and the Australian and New Zealand College of Anaesthetists Clinical Trials Network, and the Australian and New Zealand Intensive Care Society Clinical Trials Group. Restrictive versus liberal fluid therapy in major abdominal surgery (RELIEF): rationale and design for a multicentre randomised trial. BMJ Open 2017;7:e015358. doi:10.1136/bmjopen-2016-015358
Myles PS, McIlroy DR, Bellomo R, Wallace S. Importance of intraoperative oliguria during major abdominal surgery: findings of the RELIEF Trial. Br J Anaesth 2019; 122:726-733.
Gurunathan U, Rapchuk IL, Dickfos M, Larsen P, Forbes A, Martin C, Leslie K, Myles PS. Association between obesity and septic complications in major abdominal surgery: secondary analysis of the RELIEF randomized clinical trial. JAMA Network Open 2019; 2:e1916345. doi:10.1001/jamanetworkopen.2019.16345